As part of our Stroke Visionaries interview series, we had the pleasure of speaking with Dr. Wendy Dusenbury.
Dr. Wendy Dusenbury is a Nurse Practitioner and Stroke Specialist whose career has spanned rural family practice, neurosurgery, neurocritical care, mobile stroke units, and telestroke. She completed her nursing degree at Northwestern Oklahoma State University, later earning her MSN and FNP from Wichita State University, a DNP from the University of Alabama at Birmingham, a post-master’s acute care certificate from the University of Nebraska, and a PhD from the University of Tennessee. She completed a neurovascular fellowship from Health Outcomes Institute and is board certified as an Advanced Neurovascular Practitioner (ANVP). Dr. Dusenbury has helped build comprehensive stroke systems in Kansas, Tennessee, and now Arizona, and is deeply involved in stroke education, rural outreach, and research in post-stroke sexual dysfunction.

Thank you so much for joining us in this interview series! Before we dive in further, could you tell us a bit about your personal journey? What sparked your interest in medicine, and what led you to where you are today?
Dr. Dusenbury: I grew up in Kansas and completed my nursing degree in a small state college in Oklahoma. After my husband and I married, we lived in western Kansas, where I worked in home health and did some administrative work. I knew I wanted to do something different, so I started looking at options. In nursing school, a nurse practitioner had come to talk to our class; at that time, nurse practitioners weren’t very widely utilized and were mostly in primary care, but I remember thinking, “That really sounds cool.” A few years later, we moved near Wichita, I saw that Wichita State had grants for nurse practitioner training, so I went back and chose the family practice track. My first job was in a rural health clinic, which was a great learning experience but not quite what I was looking for. I then moved to a large pediatric practice in Wichita, where I worked for several years with excellent physicians and learned a tremendous amount.
The Fluidity of the Nursing Path(s)
You’ve worked in a few different specialties: pediatrics, neurosurgery, and neurocritical care. How did stroke become your focus?
Dr. Dusenbury: One of the beautiful things about nursing is that you’re not restricted to one path; if you need to change it up, you can. After pediatrics, I was recruited into neurosurgery and spent a couple of intense years in the operating room, which was an incredible learning experience. Later, I took a role in neurocritical care and thought my neurosurgery background would carry me, but we started responding to stroke alerts in the emergency department and I realized I knew nothing about stroke. That was a turning point. I started looking for ways to learn about stroke and found an advanced practice stroke fellowship that I could do remotely. Through that fellowship I connected with stroke leaders at UAB, helped our hospital work toward comprehensive stroke center status, and eventually completed my DNP with a focus on stroke. That is really when stroke became my home.
Telestroke, and Mobile Stroke Units in Memphis
You have worked on mobile stroke units and helped design a telestroke program. What did that look like in practice and how was the experience?
Dr. Dusenbury: After my stroke fellowship and DNP, I was teaching full time and still working clinically when I was recruited to help start a mobile stroke unit in Memphis. I lived in Wichita at the time, but we worked it out so I would travel back and forth every other week. It was a wild experience; on a mobile stroke unit there is no telling what you are going to encounter, but it is an incredible way to bring stroke care directly to patients.
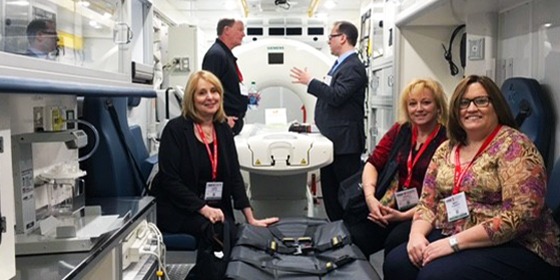
Around the same time, our health system in Memphis had one comprehensive stroke center and four primary stroke centers. The primary centers had neurology coverage, but many were uncomfortable keeping patients who had received alteplase, so they were transferring almost everyone. We treated 1000 patients with thrombolytics in the city that year, and you can imagine the strain that put on the comprehensive center and on families. The question became: how can we stop all these transfers? We created a Nurse Practitioner-led telestroke service where we rounded daily via telemedicine on patients at the outside hospitals and were responsible for their stroke workup. At first we had one or two patients; eventually we were consistently following eight to ten, sometimes more. As the program grew, so did trust; those hospitals became more comfortable keeping appropriate patients because they knew the stroke workup was being done, and we functioned as a direct extension of the comprehensive center.
Rural Stroke Care
You’ve spent a lot of time working with rural hospitals. How do you think stroke care can be improved in rural communities?
Dr. Dusenbury: I do some work with the Kansas Clinical Improvement Collaborative, which does stroke outreach across Kansas, and I’m still involved with some of that. We go out and educate providers, nurses, and doctors on stroke care: when to give tenecteplase or tPA, what labs need to be drawn, what stroke alerts should look like, and how to prevent complications like aspiration with swallow evaluations. Those things are important, but a big problem in rural America is simply getting to care. I grew up in that environment; my dad would go to the doctor only when he thought he was severely ill. That mindset still exists in many places. We need public education so people recognize stroke symptoms and seek help quickly, and we need to support rural providers. I believe a comprehensive stroke center’s job is not only to care for its own patients but to support all the hospitals in its catchment area, whether that is by phone consultation, telemedicine, or other systems that empower rural teams to care for stroke patients locally when it is safe to do so.
Research on Hemorrhagic Stroke and Sexual Dysfunction
Some of your research focuses on hemorrhagic stroke and sexual dysfunction after stroke, which is a topic many people avoid. What drew you to those areas?
Dr. Dusenbury: My dissertation work focused on hemorrhages, and I remain very interested in hemorrhagic stroke. There has been little found to truly help patients with this kind of stroke and there is a huge opportunity to improve survival rates and meaningful outcomes. I also have a special interest in sexual dysfunction after stroke, which I sort of stumbled into. While teaching at Wichita State, I had a colleague whose area of expertise was sexual dysfunction and heart failure, and as a new faculty member on the tenure track I needed publications and did not feel very prepared. She mentored me, and that work started there. It went dormant for a while and then picked back up. I authored a topical review that was published last spring in Stroke on post-stroke sexual dysfunction. We know that 50 to 70 percent of patients will have some sort of sexual dysfunction after stroke, and it is directly linked to depression, but the big problem is that nobody asks. Clinicians feel uncomfortable, they don’t want to embarrass people, and we also do not have great assessment tools built into routine stroke care. I am interested in creating ways for patients to disclose these issues more comfortably, possibly with questionnaires they can complete outside of a face-to-face encounter, because it is a huge quality-of-life issue that we are not addressing.
Giving Back
You are heavily involved in organizations like the Association of Neurovascular Clinicians (ANVC) and the American Heart Association (AHA), all while continuing to balance family and clinical work. What gives you the energy to continue giving back?
Dr. Dusenbury: I have been involved with the Association of Neurovascular Clinicians nearly since its beginning. With ANVC, it has been incredibly fun to watch the organization grow, to see people you helped bring into the circle or mentored in some small way really excel and become the next generation of leaders that drive progress forward. I think you have to decide what is important to you personally and what you are willing to put your energy into. For me, that community, and the chance to see others flourish, is a big part of what keeps me engaged.
The same spirit carries through to my work with the American Heart Association, where I am active in the Cardiovascular and Stroke Nursing Council and currently chair the Stroke and Neurovascular Committee.

What would you say to the next generation who are considering a career in stroke or advanced practice neurology?
Dr. Dusenbury: I often tell people to think about what gives them purpose. There are days when you go home and ask, “What am I doing?” and there are days when you know that if you had not been there, a patient would be completely disabled. Those are the moments that fill you back up. You have to figure out what fills your time and what fills your soul, and then learn how to balance the two. Stroke can be demanding, but it can also be incredibly rewarding when you see the difference you make.
If you or someone you know is driving change in stroke care, we’d love to hear from you. Please send an email with your nomination to Emma Houtz at ehoutz@brainomix.com.
Stay tuned for more editions of Stroke Visionaries.